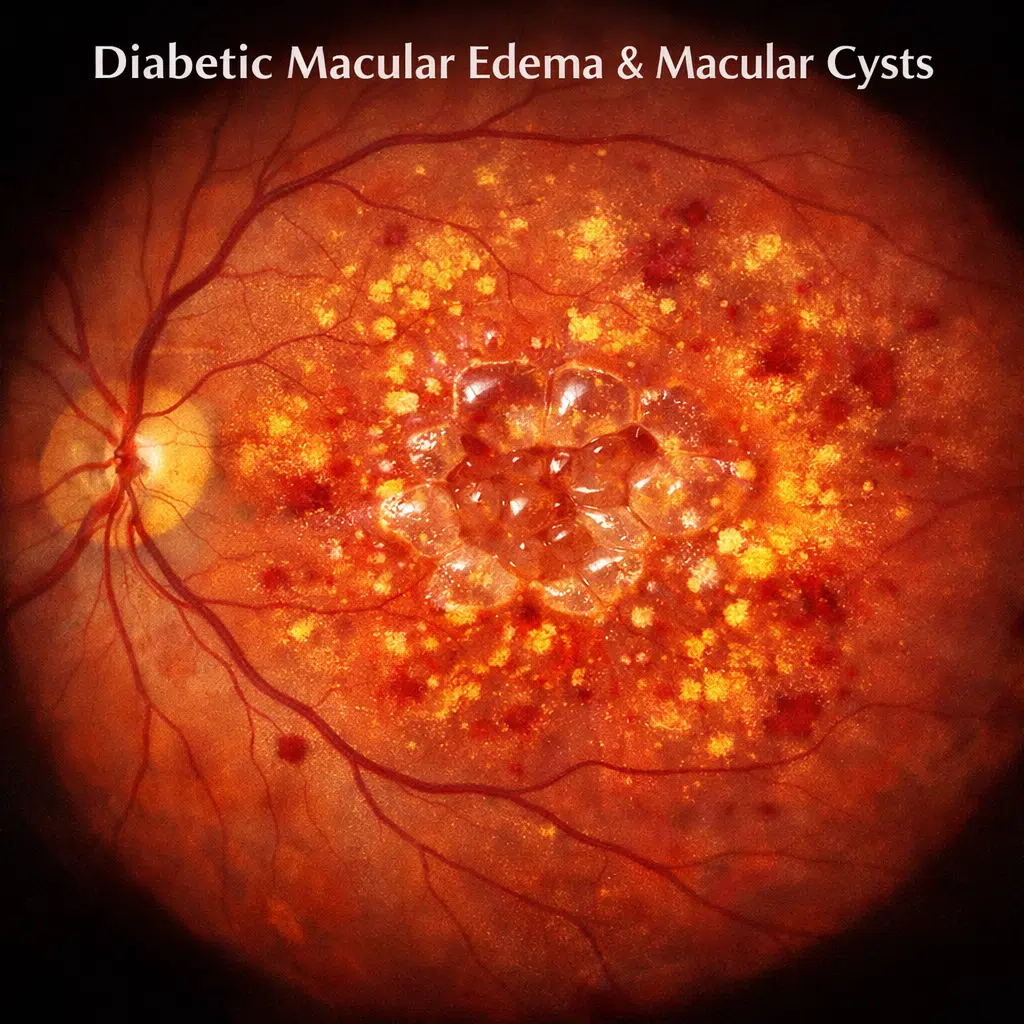
Receiving a diagnosis related to your vision can feel overwhelming, especially when terms like macular cysts or cystoid macular edema are mentioned alongside diabetes. You might worry about what these terms mean for your sight, your independence, and your future. It is completely normal to feel this way.
The good news is that these terms often sound more frightening than they actually are. In many cases, they describe specific patterns of swelling in the macula that doctors understand well and can treat effectively. In fact, Population studies show that approximately 4–7% of people with diabetes develop diabetic edema macular, making it a common and well-studied complication (DME), making it a relatively common and well-studied complication rather than a rare or untreatable condition.
My goal is to help you understand your eye health in a clear and simple way so you can make decisions with confidence. We will break down what these conditions are, why they happen, and most importantly, how they can be managed to help you protect your vision.In this guide, we will explore the relationship between diabetic macular edema and macular cysts, look at the symptoms you might experience, and walk through the treatment options available to you.
Understanding the Difference: Macular Cysts vs. DME
When your eye doctor mentions “macular cysts,” “cystoid changes,” or “cyst-like spaces,” it can sound like you have developed a completely new or separate disease. However, these terms usually describe a specific pattern of swelling rather than a different diagnosis.
To understand what is macular edema better, let’s clarify two main terms
- 1. Diabetic Macular Edema (DME): This refers to diabetic macular edema, caused specifically by diabetes. When blood sugar levels are high over time, they can damage the tiny blood vessels in the retina, leading to diabetic macular edema. This damage leads to fluid leaking out, causing the macula (the center part of the retina) to swell.
- 2. Cystoid Macular Edema (CME): This describes a specific appearance of that swelling. Instead of general puffiness, the fluid collects in small pockets, forming a honeycomb-like or “cystoid” pattern within the retina.
1. The Relationship Between DME and CME
It helps to think of what macular edema is- as the “what” (swelling caused by diabetes) and CME as the “how” (how that swelling looks on a scan).
When you have diabetic macular edema, the fluid often organizes itself into these cyst-like pockets. So, if your doctor says you have cystoid macular edema, they are usually describing the specific shape your diabetic swelling has taken.
A helpful comparison:
- 1. DME (Diabetic Macular Edema): The cause is always diabetes. It affects the blood vessels in the retina.
- 2. CME (Cystoid Macular Edema): The appearance is like small fluid pockets. While diabetes is a common cause, it can also happen after cataract surgery or due to other eye conditions.
Why does this distinction matter? Understanding that “macular cysts” are often just a feature of your diabetic macular edema can be reassuring. The underlying issue is still the diabetes-related leakage, meaning the treatment plan remains focused on managing the DME and controlling your blood sugar.
| Feature | DME | CME |
| Definition | Diabetes-caused retinal swelling | Cyst-pattern swelling (fluid pockets) |
| Cause | Always diabetes | Multiple causes, including post-surgical issues or other eye conditions |
| Appearance on OCT | Variable patterns | Honeycomb or petaloid cyst-like spaces |
| Layers Affected | Multiple retinal layers can be involved | Primarily inner nuclear and outer plexiform layers |
2. Common Causes of CME
Common causes of CME include cataract surgery (the most common cause), diabetic macular edema (DME), retinal vein occlusion, uveitis, and certain medications.
- 3. Why This Matters?
If you have diabetes and your doctor mentions “cystoid changes” or “macular cysts,” they are usually describing the pattern of diabetic macular edema.
- 1. Even though it may look like cysts, the main cause is still diabetes-related swelling and fluid leakage.
- 2. This means treatment will focus on managing DME and keeping your diabetes under control.
Macular Cysts Explained
Let’s look a little closer at what macular cysts actually are. Despite the name, these aren’t “true” cysts like you might find elsewhere in the body, which have a distinct wall or lining. Instead, macular cysts are pockets of fluid that push retinal cells apart.
Imagine a sponge soaking up water. As it swells, gaps or spaces form within the sponge’s structure. Similarly, when the retina swells, fluid accumulates between the layers of retinal cells. On an imaging scan called an OCT (Optical Coherence Tomography), these fluid-filled spaces appear as dark circles or ovals, often described as a macular retinal cyst.
- 1. What are Macular Cysts?
Macular cysts are fluid-filled spaces within the retina, typically located in specific retinal layers. Although termed “cystoid,” they are not true cysts with a distinct wall or lining. Instead, they are pockets of fluid that accumulate between retinal cells. On Optical Coherence Tomography (OCT) imaging, these cyst-like spaces appear as dark or black circular or oval areas. Macular cysts most commonly occur in the inner nuclear layer (INL) and the outer plexiform layer (OPL) of the retina.
- 2. Why Do These Cysts Form?
Your retina has a built-in system to keep itself dry and functioning well, known as the blood-retinal barrier. When this barrier is damaged, often by high blood sugar levels, one of the main retinal swelling causes the tiny capillaries (blood vessels) become leaky.
- a. Leakage: Damaged capillaries leak fluid and proteins into the retina.
- b. Accumulation: The retina’s pump system cannot clear the fluid fast enough, so it builds up.
- c. Distortion: This fluid pushes normal retinal structures apart, forming macular cysts.
This swelling distorts the shape of the macula, which is responsible for your sharp, central vision and leads to diabetic macular edema symptoms. These changes are part of the common macular edema signs and symptoms, which often include blurry or wavy vision.
3. How OCT Imaging Shows Macular Cysts?
Your doctor uses optical coherence tomography (OCT) to detect macular cysts. On an OCT scan, macular edema on OCT appears as dark circular or oval spaces within the retina. Often, they are arranged in a pattern resembling a honeycomb or flower petals, making them easily identifiable. This imaging technique helps your doctor assess the extent of fluid buildup and plan appropriate treatment.
4. Types of Macular Cysts
Doctors categorize these cysts based on where they are and what they look like.
- a. Inner Retinal Cysts: These are found in the inner layers of the retina and are very common in diabetic macular edema.
- b. Outer Retinal Cysts: Found deeper in the retina, these are less common and can sometimes indicate that the swelling has been there for a longer time.
- c. Subretinal Fluid: Sometimes fluid builds up under the retina. It isn’t technically a cyst, but it often occurs along with them.
5. By Appearance
- 1. Focal Cysts
These are isolated pockets of fluid within the retina. - 2. Diffuse Cystoid Spaces
Widespread cyst-like spaces scattered across the macula often indicate more widespread damage. - 3. Large Cysts
These are larger fluid pockets, often associated with poorer visual outcomes due to their size and underlying damage.
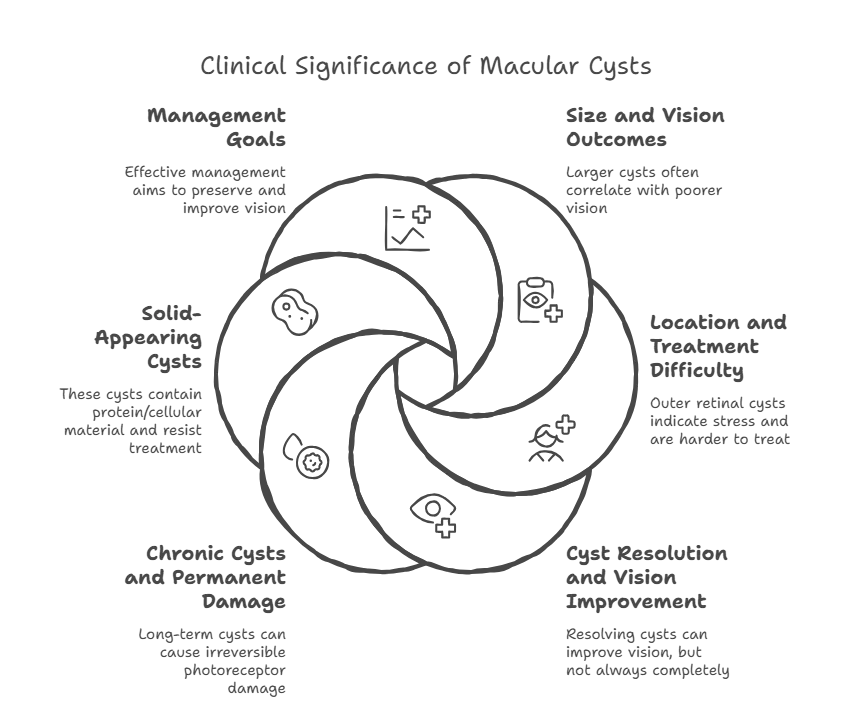
6. Clinical Significance
Doctors carefully monitor cysts because they provide insight into retinal health and potential vision recovery:
- a. Larger cysts are often linked to worse vision outcomes.
- b. Outer retinal cysts may indicate greater retinal stress and are typically harder to treat.
- c. Cyst resolution can lead to improved vision, though recovery may not always be complete.
- d. Chronic cysts can cause permanent photoreceptor damage, limiting recovery even if swelling reduces.
- e. Solid-appearing cysts are a special case where cysts are filled with protein or cellular material instead of clear fluid. These are typically more resistant to anti-VEGF treatments and may indicate long-standing retinal damage.
Managing these cysts effectively is key to preserving and improving vision.
Your doctor pays close attention to the size and location of these cysts. Larger cysts are often linked to more significant vision changes. However, when a macular retinal cyst resolves with treatment, vision often improves, which gives us a clear goal to work toward.
Causes of Macular Cysts (Beyond Diabetes)
While diabetes is a major cause, it is helpful to know that macular cysts can develop from other conditions, too. If you have diabetes, your doctor will likely suspect diabetic macular edema first. However, if you have recently had eye surgery or other eye issues, those factors could be contributing.
Here are other common causes of cystoid macular edema:
- 1. Post-Cataract Surgery: This is one of the most common causes of retinal swelling cysts in people without diabetes. It typically happens a few weeks after surgery and is often treated with anti-inflammatory drops.
- 2. Retinal Vein Occlusion (RVO): A blockage in a retinal vein can cause blood and fluid to back up into the retina, causing severe retina swelling.
- 3. Uveitis: This is an inflammation inside the eye. Chronic inflammation can break down the barriers in the eye, leading to macular cyst formation.
- 4. Wet Age-Related Macular Degeneration (AMD): Abnormal blood vessels grow under the retina and leak, sometimes causing cyst-like changes.
- 5. Medications: Certain eye drops (like those for glaucoma) or other medications can sometimes trigger macular cysts.
- 6. Retinitis Pigmentosa: In later stages of this genetic condition, cysts can form in the macula.
It is possible to have more than one cause at the same time. For example, if you have diabetes and recently had cataract surgery, your macular edema therapy might need to address both the surgery-related inflammation and the diabetes-related leakage.
Symptoms Specific to Cystoid Changes (Macular Cysts)
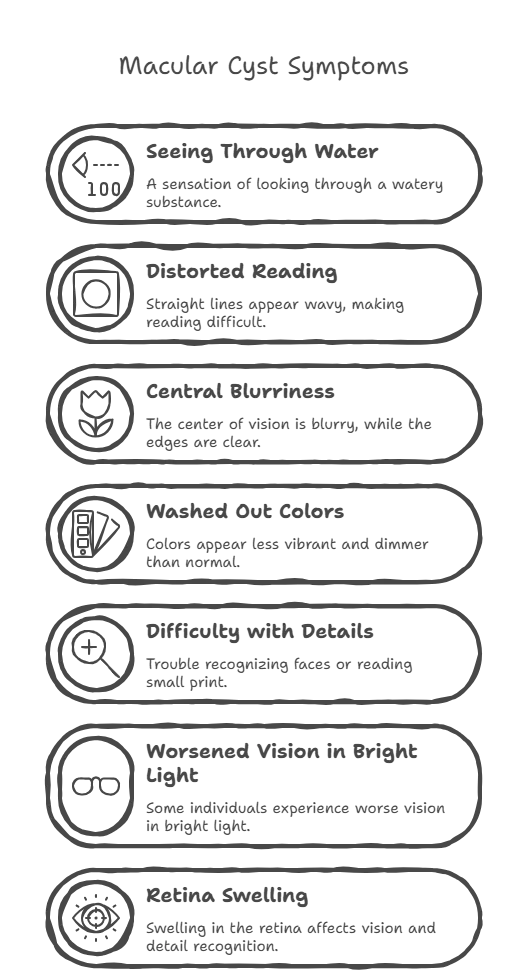
Macular cysts can alter how light is focused in the center of your vision, leading to diabetic macular edema symptoms that impact daily life. These effects are among the most noticeable macular edema signs and symptoms people experience. Common symptoms include:
- a. A “seeing through water” sensation.
- b. Distorted reading, where straight lines appear wavy (metamorphopsia), is one of the classic macular edema symptoms.
- c. Central blurriness is one of the most common macular edema symptoms, while peripheral vision often remains relatively clear.
- d. Colors may appear washed out or dimmer than usual.
- e. Difficulty with fine details, such as recognizing faces or reading small print and phone text.
- f. Worsened vision in bright light for some individuals.
- g. Retina swelling. Difficulty with fine details, such as recognizing faces or reading small print and phone text, is common with retina swelling symptoms.
The severity of vision loss often correlates with the size and location of the cysts. A central subfield thickness above 400 microns generally results in noticeable symptoms. Cysts that affect the foveal center are linked to the most severe loss of vision.
Diagnosing Macular Edema and Cysts
To confirm if you have diabetic macular edema or macular cysts, your doctor will use specialized imaging. The most common and important tool is the OCT scan.
- 1. OCT (Optical Coherence Tomography)
Optical coherence tomography (OCT) is a key tool for identifying and managing macular cysts. It uses light to create detailed, cross-sectional images of the retina, showing macular edema on OCT through fluid accumulation and retinal layers. OCT helps doctors assess:
- Central subfield thickness (normal range: 250-280 microns)
- Cyst size, number, and location
- Photoreceptor layer integrity, which affects vision prognosis
- Subretinal fluid presence
- Surface changes, such as epiretinal membrane or vitreomacular traction
DME classification by OCT:
- Center-involved DME (ci-DME): Cysts or thickening within the central 1 mm zone
- Non-center-involved DME: Cysts or thickening outside the central 1 mm zone
- Swelling patterns (focal vs diffuse)
- Appearance (cystoid vs non-cystoid)
Monitoring with OCT is vital. Doctors use macular edema on OCT to track changes, including cyst size, fluid resolution, and response to treatment. OCT scans are often repeated during visits to monitor progress or detect new swelling areas. This non-invasive imaging is essential for managing diabetic macular edema and guiding treatment decisions.
- 2. Fluorescein Angiography
Sometimes, your doctor might order a test called fluorescein angiography. This involves injecting a special dye into your arm, which travels to your eye. A camera takes pictures as the dye moves through your retinal blood vessels. This test shows exactly where the leakage is coming from, whether it is specific leaking spots (microaneurysms) or a general leakage area associated with diabetic edema macular.
Treatment Options for Macular Cysts and DME
The presence of cysts on your scan doesn’t change the main goal of treatment: to dry up the fluid and stabilize your vision. Treating diabetic macular edema with appropriate macular edema therapy usually resolves the cysts because they are just a symptom of the swelling
Here are the primary diabetic macular edema treatments your doctor may recommend:
1. Anti-VEGF Injections (The Gold Standard for diabetic macular edema treatments)
This is the most common and effective treatment for macular edema. Medications like Eylea, Lucentis, Vabysmo, and Avastin are injected into the eye to block a protein called VEGF. This protein causes blood vessels to leak.
- How it works: By blocking VEGF, the medication stops the leakage. As the leakage stops, the fluid absorbs, and the macular cysts shrink or disappear.
- What to expect: It often takes a series of injections to see results. Your doctor might start with monthly injections and then extend the time between visits as your eye stabilizes.
- Results: Many patients see significant improvement in macular edema symptoms and a reduction in cysts on OCT scans.
2. Steroid Implants or Injections
If anti-VEGF injections aren’t fully effective, or if inflammation is a major factor, your doctor might suggest steroids.
- How it works: Steroids are powerful anti-inflammatories that reduce swelling and leakage.
- Options: Long-acting implants (like Ozurdex or Iluvien) release medication slowly over months or years.
- Considerations: Steroids can increase the risk of cataracts or high eye pressure, so your doctor will monitor you closely.
3. Laser Treatment
While less common now due to the success of injections, laser therapy is still used in specific cases. Focal laser treatment can seal off specific leaking blood vessels. It is often used to stabilize vision rather than restore lost sight.
4. Surgery (Vitrectomy)
In rare cases, the jelly inside the eye (the vitreous) pulls on the macula, preventing the swelling from going down. Surgery to remove this jelly can relieve the pressure and help the retina swelling resolve.
Living with DME and Protecting Your Vision
Managing diabetic macular edema with consistent macular edema therapy is a marathon, not a sprint. It requires patience and consistency. While medical treatments are crucial, your daily habits play a massive role in how well your eyes respond to macular edema therapy.
- 1. The Importance of Blood Sugar Control
Your hemoglobin A1c (a measure of average blood sugar) is directly linked to your eye health. High blood sugar damages blood vessels, fueling the cycle of leakage and macular cysts
- Better Control = Better Outcomes: Studies show that patients with lower A1c levels often respond better to injections and have more stable vision over time.
- Stability: Avoiding large spikes in blood sugar can help prevent retinal swelling caused by triggering a recurrence.
- 2. Adapting to Vision Changes
If you are dealing with retina swelling symptoms like blurriness or distortion, everyday tasks can feel frustrating. However, there are tools to help you maintain your independence.
- Lighting: Good lighting makes a huge difference. Use bright, direct task lighting for reading or cooking.
- Magnification: Simple handheld magnifiers or digital magnifiers can help with small print.
- Contrast: High-contrast settings on your phone or computer can make text easier to read.
- Audio: Audiobooks and voice-to-text features are great alternatives when your eyes feel tired.
- 3. Emotional Well-being
Vision loss can be emotionally draining. It is okay to feel frustrated or anxious. Support groups for people with low vision or diabetes can be incredibly helpful. You are not alone in this journey, and sharing your experience with others who understand can lighten the load.
Prognosis: What Can You Expect?
The outlook for people with diabetic macular edema and macular cysts is generally positive, especially with modern treatments.
- a. Treatment Success: About 60–70% of patients see a significant improvement in their vision with consistent anti-VEGF therapy.
- b. Cyst Resolution: With treatment, macular cysts often shrink or disappear entirely. Even if some small cysts remain, many people maintain functional vision that allows them to drive and read.
- c. Early is Better: The sooner you start macular edema treatment, the better the outcome. Chronic swelling can lead to permanent damage, so timely intervention is key.
Remember, “success” looks different for everyone. For some, it means returning to 20/20 vision. For others, it means stabilizing vision so it doesn’t get worse. Both are victories.
How Soon After Treatment Will I Be Able to Get Back to Work or School?
If you’re planning your schedule around eye treatments for macular edema or cysts, you might be wondering how much downtime to expect.
The good news is that for common treatments like anti-VEGF injections, most people can return to work or school the very next day and sometimes even the same afternoon.
Here is a simple guide to help you plan your recovery:
The Day of Your Treatment
It is completely normal for your vision to feel a little blurry or “gritty” for a few hours. This is usually just a reaction to the antiseptic drops or the injection itself. You might also notice your eye looks a bit red.
While you don’t need to stay in bed all day, many of my patients prefer to take it easy for the rest of the afternoon. Listen to your body and rest if you need to.
The Next Day
Most people feel comfortable getting back to their normal activities by the next morning. This includes:
- a. Office work
- b. Going to school
- c. Reading
- d. Using screens (like phones or TVs)
You might be a little sensitive to bright lights at first, but this usually improves quickly.
A Note for Physically Demanding Jobs
Does your work involve heavy lifting, intense physical strain, or dusty environments? If so, I usually recommend waiting 24 to 48 hours before heading back. This gives your eye a chance to settle and reduces the risk of irritation or infection.
Jobs That Require Sharp Focus
If your daily tasks require perfect central vision, like driving, reading fine print, or detailed technical work, you may need a little more patience.
Even though you are physically capable of working, your vision depends on how quickly the swelling in your eye goes down. This can sometimes take weeks or months. Be gentle with yourself during this process.
Recovering from Implants or Surgery
If you have had a steroid implant or a surgical procedure, your recovery road might be slightly longer. Your doctor will give you specific steps to follow, especially regarding eye pressure, so be sure to follow their guidance closely.
Frequently Asked Questions
Q1: What is the difference between macular edema and a macular cyst?
A: It is the general swelling of the macula. A macular cyst or macular retinal cyst describes the specific pattern that swelling takes, forming pockets of fluid. Essentially, edema is the condition, and cysts are how it looks.
Q2: Can macular cysts go away on their own?
A: It depends on the cause. Cysts from cataract surgery sometimes resolve on their own. However, macular cysts caused by diabetes usually require treatment to dry up the fluid and prevent damage.
Q3: Is a macular cyst the same as a macular hole?
A: No. A macular cyst is a fluid-filled space within the retinal layers. A macular hole is an actual break or gap in the center of the retina. They are different conditions with different treatments.
Q4: Can stress cause swelling on the retina?
A: Directly, no. However, stress raises blood pressure and cortisol levels, which can negatively affect diabetes control. Poor diabetes control is a leading cause of swelling on the retina. Central Serous Chorioretinopathy is another condition sometimes linked to stress that causes fluid under the retina, but it is different from DME.
Q5: How long does it take for macular edema to clear up?
A: Many patients see improvement within 2–3 months of starting injections. However, complete resolution of macular cysts can take longer, and some chronic cysts may not fully disappear even if vision improves.
Taking the Next Step
Hearing terms like macular cysts or diabetic macular edema can be scary, but remember that these are treatable conditions. They are not a sentence for blindness. By working with your eye doctor, keeping up with your appointments, and managing your diabetes, you are taking powerful steps to protect your sight.
If you have noticed changes in your vision or are struggling with daily tasks, don’t wait. Reach out to your eye care specialist. There is hope, there is help, and there are effective treatments available to help you keep seeing the world clearly.