Typical expenses:
How Much Do Injections For Macular Degeneration Cost? Out-of-pocket expenses for consumers with health insurance often include copays for doctor visits, copays for prescription drugs, or coinsurance of 10% to 50%. Insurance often pays for macular degeneration treatment.
A two-year course of therapy with medications injected into the eye to suppress the production of and leakage from extra blood vessels often costs individuals without health insurance between $9,000 and $65,000, depending on the drug used.
For two years of treatments with Visudyne and photodynamic therapy, which functions similarly, the cost may reach $10,000 in most cases.
Because so few individuals are suitable, laser therapy to burn leaky blood vessels is done far less often; it normally costs about $1,700; it frequently has to be repeated, and the surgery itself may result in vision loss.
A vial of the brand-name cancer drug Avastin costs about $50, or about $1,200 for monthly injections over the two years typically required, while a vial of the brand-name drug Lucentis costs about $2,000, or about $48,000 for monthly injections over the two years typically required.
Doctors also charge. This is according to the American Macular Degeneration Foundation. For instance, Midwest Eye Care in Nebraska bills $380 for a single Avastin treatment, or $9,120 for monthly treatments over the course of two years. A Visudyne injection with photodynamic therapy (PDT) costs roughly $2,000 for each session, or a total of $10,000 for five treatments spaced out over two years, according to Retinal Consultants of San Antonio in Texas. Additionally, one Macugen treatment costs roughly $1,250, or more than $21,000 for treatments every six weeks for two years, according to Retinal Consultants of San Antonio. One Lucentis treatment costs $2,700 at Midwest Eye Care.
What does AMD treatment consist of?
A doctor may advise using an Amsler grid to check eyesight at home if you have dry macular degeneration.
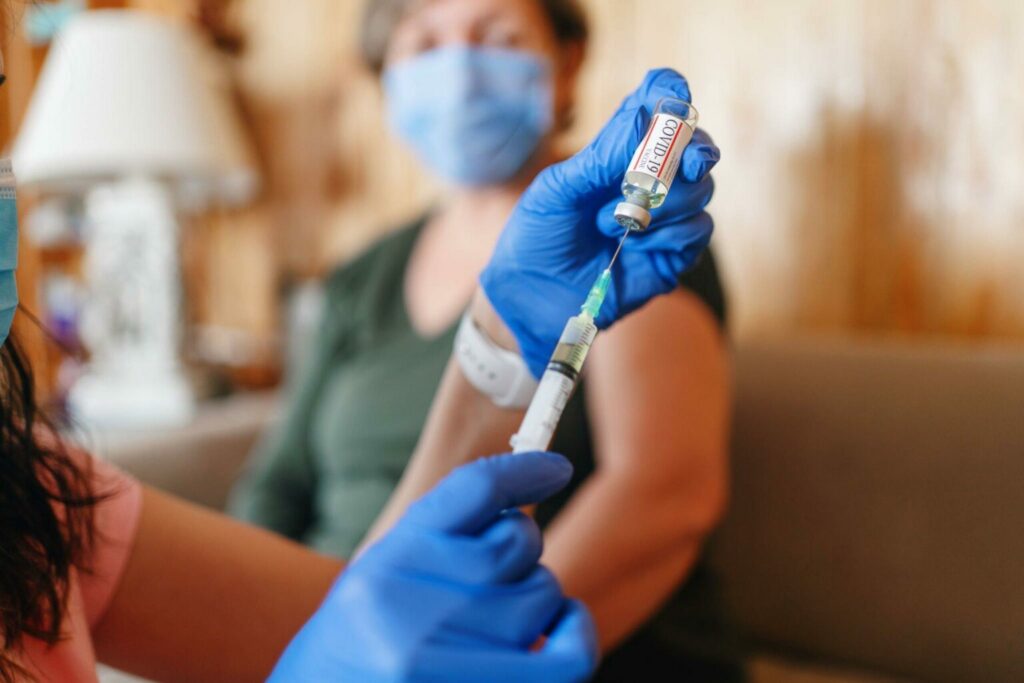
A doctor may recommend injections into the eye using bevacizumab (brand name Avastin), a chemotherapy medicine that is used off-label, pegaptanib (brand name Macugen) or ranibizumab (Lucentis) for wet macular degeneration, in which a cluster of leaky blood vessels grows in the eye. All three medications prevent the growth and leaking of blood vessels. Depending on the medicine, injections are normally needed every month to every six weeks for roughly two years.
The physician may advise using photodynamic therapy in conjunction with verteporfin (Visudyne) (PDT). Typically, a doctor will inject the medication into a vein in the body, and then flash a specific wavelength of light into the patient’s eye, causing the medication to constrict the blood vessels in the eye. There may be a need for more treatments, often every three months.
A physician uses a laser during laser photocoagulation to burn and shut off blood arteries; this procedure often calls for a local anesthetic. This therapy has a number of disadvantages and can only be utilized in roughly 15% of instances, according to WebMD.
Additional expenses for AMD Treatment
Patients with early-stage AMD may be able to delay the disease’s development by taking certain antioxidants and zinc, according to a National Eye Institute study. For a three-month supply, supplements created based on the research cost between $15 and $30.
Cash discounts and support programs:
For uninsured or cash-paying individuals, many hospitals and physicians provide discounts of up to 30% or more. For instance, the Californian Washington Hospital Healthcare System[17] provides a 35% discount.
Some pharmaceutical companies have patient support programs. Together Rx Access is a discount card that provides 25%–40% off various brand-name medications for patients without prescription drug coverage who are also ineligible for Medicare. The majority of businesses also provide customers without insurance who satisfy specific requirements with free medications.
How many eye injections for macular degeneration
Anti-VEGF, or anti-vascular endothelial growth factor, medications must be injected into the eye on a monthly or biweekly basis to treat wet AMD. Anti-VEGF medications may, in most circumstances, successfully halt future vision loss while slowing or stopping the formation of blood vessel leaks. But for many patients, the need to visit a doctor’s office or clinic every month for injections is a barrier to care, resulting in missed treatments and perhaps deteriorating eyesight.
Up to 30% of patients with wet macular degeneration might safely stop receiving eye injections, according to a recent study.
Researchers are developing a quick test that might one day determine whether patients can quit receiving treatment.
According to a pilot study of 106 patients with “wet” age-related macular degeneration, up to one-third of individuals with the debilitating retinal condition may one day be able to discontinue receiving eye injection treatment without suffering additional vision loss. The data, according to the researchers (From the John Hopkins School of Medicine ), do not provide a timetable for stopping therapy or an exact list of individuals who can cease injections, but they do add to mounting evidence that many people with the condition may not need the lifetime monthly medicine that is presently advised.
The results, according to the researchers, also indicate certain proteins generated at various quantities in the eyes of individuals who discontinued treatment, which might result in the creation of a test to precisely determine which patients can safely be weaned off medicine.
Are eye injections for macular degeneration painful?
The injection often causes little discomfort. Some folks experience some pressure or discomfort. You can see wavy lines when the anti-VEGF combines with the fluid in the center of your eye.
Once the needle is removed, your doctor will apply pressure to the injection site with a sterile cotton tip for approximately 10 seconds to prevent fluid leakage. Your eye will then be flushed with a substance to lubricate it and prevent irritation.
Follow-up period
Within a week following your injection, your wet AMD symptoms may start to improve. After the injection, you can feel uncomfortable for a few days and your eyesight might be a little blurry. To ease the soreness, you may use over-the-counter painkillers like acetaminophen or ibuprofen. You might also ease pain by placing a cold washcloth over your eyes for approximately ten minutes every half-hour.
You could have some redness in the whites of your eyes for up to two weeks if the needle your doctor used accidentally poked a blood vessel in your eye. This is a benign side effect as long as there is no discomfort or visual issues.
Inform your doctor if you have any adverse effects after your injection so that you may come in for an eye exam. Here are some signs to look out for:
- Eye discomfort
- Light sensitivity
- Distorted vision
- Increased pressure
- “Floaters” in your line of sight
Infection symptoms include pain, sensitivity to light, and changes in vision. Although these side effects are uncommon, you should let your eye doctor know if you experience them or any of the symptoms mentioned above.
Do eye injections help macular degeneration?
The retina’s buildup of cellular waste products, which prompts it to start producing new blood vessels, causes macular degeneration. Doctors may assist a patient to maintain their eyesight by injecting drugs that prevent the development of new blood vessels.
The retina’s surplus cellular waste eventually fosters the growth of new blood vessels. It transforms into exudative or “wet” macular degeneration when they appear. The blood vessels are very tiny and fragile and can break or rupture causing leakage. Without therapy, the retinal tissue may become scarred and these new blood vessels may bleed readily, leaving the patient legally blind.
The presence of a protein called (VEGF) vascular endothelial growth factor causes wet macular degeneration. Blood vessel growth is aided by VEGF. An excessive amount of VEGF leads to the development of too many blood vessels surrounding the macula in persons with wet macular degeneration.
How do anti-VEGF injections work?
Intravitreal injections are one way that doctors may treat wet macular degeneration. Doctors administer these injections into the vitreous, a region close to the retina in the rear of the eye.
Using a needle to inject anti-VEGF drugs into the patient’s eye, these drugs work by lessening the power of VEGF, which helps stop the condition from becoming worse.
There is convincing evidence that patients with wet macular degeneration who receive these intravitreal injections may delay some visual loss. Compared to 50–60% of individuals who do not get this therapy, only 20–30% of wet macular degeneration patients who receive these injections will lose at least six lines of vision.
How effective are injections for macular degeneration?
The use of intraocular (into the eye) injections to treat wet macular degeneration has been shown effective in clinical tests. In comparison to individuals who did not opt for intraocular injections, after one year of intraocular treatment, eyesight improved by roughly 25–34%.
The drugs used to treat wet macular degeneration include Avastin (bevacizumab), Lucentis (ranibizumab), and Eylea (aflibercept). For almost a year, they are injected into the eye every four weeks. Your eye doctor may determine how often you need injections once a year has passed.
The continued vision loss has been found to be stopped by these injections, and in some instances, the eyesight has even improved. Starting the treatment between 7 and 21 weeks after the first symptom is when it is most beneficial.
Numerous investigations found that two years following the commencement of the therapy, gains were steady and sustained. Following therapy, multiple scans revealed the improved retinal structure and decreased scarring in the retina.
FAQ’s
Can macular degeneration be reversed with injections?
When anti-VEGF antibodies are injected into the eye, lost vision in people with wet AMD, which is brought on by new, leaky blood vessels forming in the retina, may sometimes be restored. These include ranibizumab (Lucentis®), aflibercept (Eylea®), and brolucizumab (Beovu®).
How long can you get macular degeneration eye injections?
Many patients now get injections on a monthly basis; most receive them eight times a year. These macular degeneration injections are now a lifetime continuous treatment for macular degeneration until an alternate therapy for the condition becomes available.
What should you avoid doing after eye injections?
Avoid rubbing the injected eye. For 48 hours, you shouldn’t wash your face, or hair, or take a shower. After the injection, you shouldn’t go swimming for a week. Four to eight weeks after the injection or series of injections, you will be scheduled for a follow-up visit.
After receiving an eye injection for macular degeneration, can you drive?
No, after getting an injection in your eye, you will need to have someone else drive you home. To prevent your eyes from drying out and feeling unpleasant following the injection, it is preferable to keep your eyelids closed for a couple of hours.
Can eye injections damage vision?
It’s possible to have hazy vision after having an injection. After some time, this adverse effect should stop. However, endophthalmitis, a potentially dangerous adverse effect of anti-VEGF injections, may also present as fuzzy vision. If this continues beyond what your doctor advises, be sure to let them know.
How many macular degeneration sufferers go completely blind?
Wet AMD accounts for approximately 10% of cases, but results in 90% of legal blindness.
What are the most recent macular degeneration treatments?
Two diseases that result in vision loss have been given new medication approved by the Food and Drug Administration (FDA). Wet AMD and (DME) diabetic macular edema, two of the most common causes of vision loss, are both treated with the medication Vabysmo (faricimab-svoa).
How dangerous are injections into the eyes?
The main dangers are
- Endophthalmitis or an eye infection.
- Eye inflammation
- Vitreous hemorrhage
- Retinal detachment (RD)