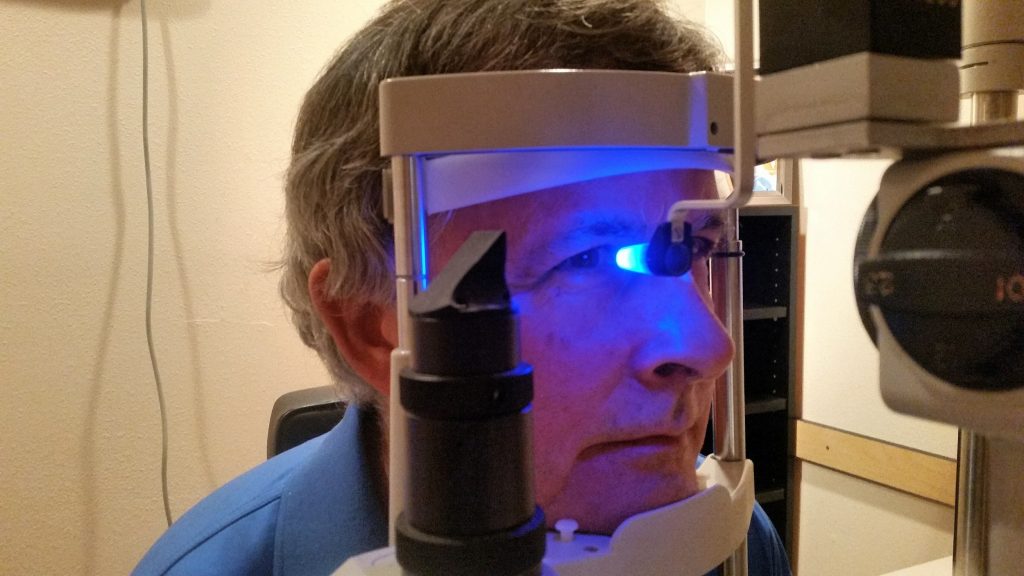
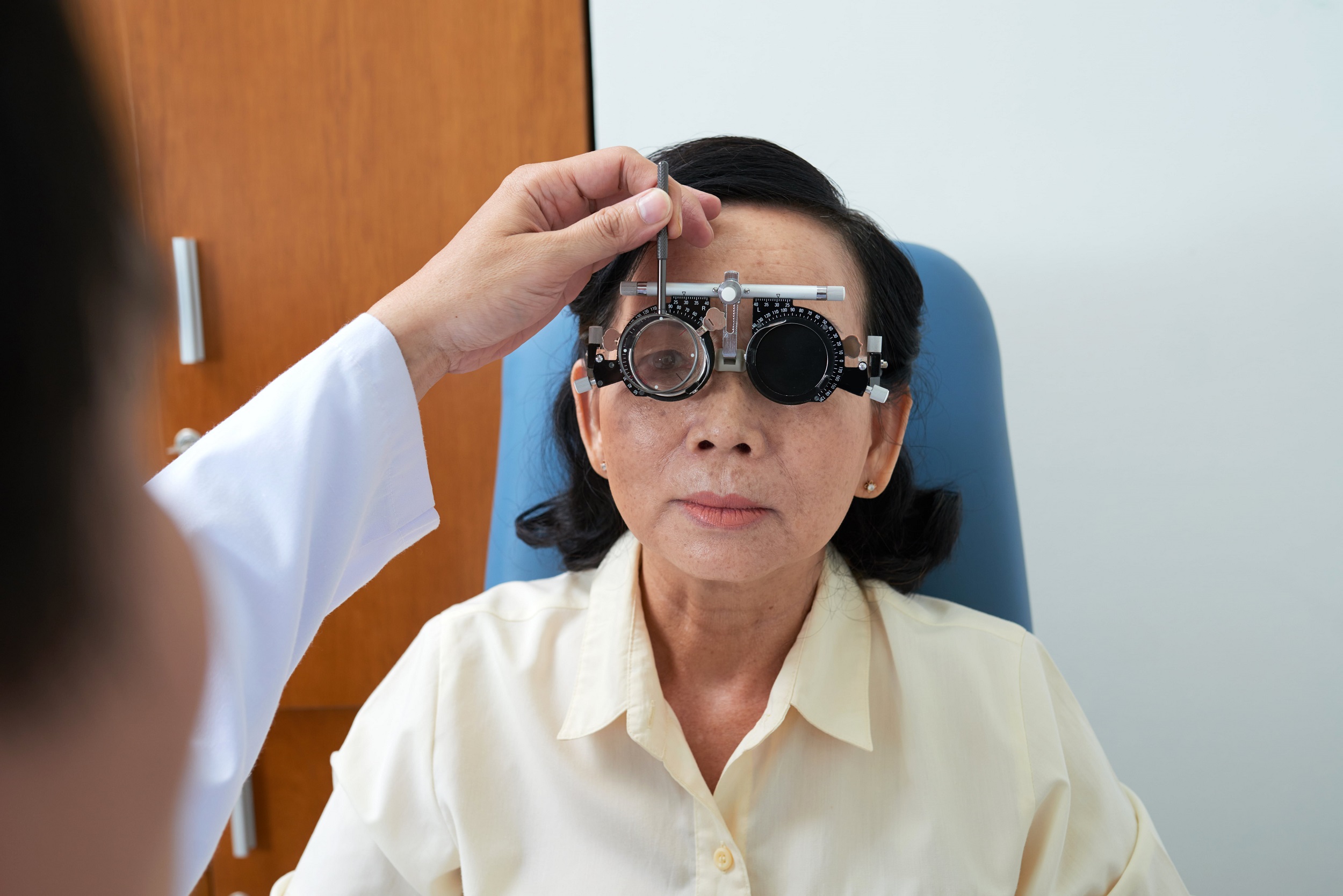
Pathophysiology, and Etiology of Transient Vision Loss (TVL) and Amaurosis Fugax
Transient vision loss in adults is a common complaint with an identified etiology in the majority of instances. The loss of vision may be unilateral or bilateral, and it can last anywhere from a few seconds to many hours.
Amaurosis Fugax and Transient Vision Loss (TVL)
Regardless of the cause, transient monocular vision loss is known as amaurosis fugax. The name amaurosis fugax, on the other hand, is better reserved for bouts of temporary monocular blindness caused by ischemia of the ocular arteries. A visual transient ischemia attack may be caused by a vertebrobasilar disruption (TIA).
Amaurosis fugax (AF) is a temporary visual loss (TVL). AF may be monocular (TMVL) or binocular (TMVL) (TBVL). Lack of oxygen to the retina, choroid, or optic nerve is the most frequent cause of monocular ischemia. TMVL is most often caused by ipsilateral carotid artery disease with subsequent thromboembolic (e.g., atherosclerosis), although it may also be a sign of vasculitis (e.g., giant cell arteritis). AF may be a sign of imminent stroke, therefore it’s important to have it checked out right away.
TBVL is rarer than TMVL and is thought to be caused by cortical lesions such as a migraine, or a seizure. Ischemic AF is a kind of transient ischemic attack (TIA), which lasts from seconds to minutes and is followed by complete visual recovery. TMVL caused by AF should be distinguished from TMVL caused by structural optic disc and intraocular causes like a retinal vein occlusion, drusen on the optic disc, or papilledema.
Overview
Temporary vision loss is a symptom, not a diagnosis. It may be caused by a variety of ophthalmic and systemic diseases, including the ones listed below:
Momentary vision impairment may be caused by transient hypoxia of any component of the visual system. Thromboembolism ( a clot), hypoperfusion ( a slowing of blood flow), or angiospasm ( a blood vessel constriction), may cause poor perfusion of the occipital lobe, visual pathways, or the eye.
Low blood pressure, heart arrhythmias, anemia, heart failure, and blood vessel plaques and arteritic cerebrovascular illness may all cause hypoperfusion. Transient vision loss may accompany artery-related anterior ischemic optic neuropathy (AAION), although it does not usually occur before nonarteritic AAION.
Adults often have temporary vision loss due to embolic occlusions of the arteries feeding the eye. Emboli that cause circulation problems may come from the heart or the carotid arteries. Because emboli are typically isolated, if visual disturbance happens often, emboli are less likely to be the cause.
Vasospasm may result in a short decrease in blood to the visual system, as well as temporary vision loss. During the brief vision loss episode, several patients underwent ocular exams that revealed obvious vasospasm on clinical examination, retinal photography, or fluorescein angiography.
Children with temporary visual loss are more likely to have a harmless disease rather than an ischemic reason for their symptoms. Migraine and, less frequently, epileptic seizures are two major causes of bilateral visual loss in youngsters. [1, 2, 3] A reason for the visual abnormality in certain youngsters has yet to be discovered, and the symptoms are medically unexplained.
Transient vision loss may run in families. In infants with induced repeated patterned daily blindness of unclear origin, several bouts of temporary visual loss have been reported. Through genetic connections such as missense mutations in SCN1A, this uncommon disease is linked to infantile epilepsy, hemiplegic migraine, and other epileptic illnesses.
Gaze-evoked amaurosis (compression) is a kind of temporary visual loss that happens when you gaze in a certain direction. Ocular surface disorders like dry eyes, foreign bodies or masses, retinal vein occlusion, central or branch retinal artery blockage, arteritic anterior ischemic optic neuropathy, intermittent angle-closure glaucoma, and optic neuritis are all possible causes of transient vision loss. Transient vision loss has also been linked to drusen and colobomas of the optic disc. The cause of temporary vision loss in these circumstances is unknown, although it may be linked to the local optic nerve or retina hypoperfusion.
After consuming a big meal, the transient visual loss has been observed. Visual loss occurs as a consequence of blood being diverted to the mesenteric system, causing hypoperfusion of the eye. Individuals whose ocular blood flow is already impaired are more likely to have a postprandial visual loss (eg, carotid disease, giant cell arteritis).
The Uhthoff phenomenon, also known as transient vision loss during exercise, is caused by increased heat exposure, which causes reduced nerve conduction via demyelinated nerves like in multiple sclerosis. Exercising may potentially induce pigment dispersion syndrome or lenticular (dislocation/subluxation) problems, resulting in temporary visual loss.
Regardless of the cause, transient monocular vision loss is known as amaurosis fugax. The name amaurosis fugax, on the other hand, is better reserved for bouts of temporary monocular blindness caused by ischemia of the ocular arteries. A visual transient ischemia attack may be caused by a vertebrobasilar disruption (TIA).
Aura migraine is a frequent source of temporary visual disruption in people of all ages. The most frequent cause of organic temporary visual loss in children is migraine. In a study of 83 individuals under the age of 45 who had episodic vision loss, migraine was shown to be the most common cause in most instances. Recurrent migraine headaches affect 3.5-5 percent of children; however, only 18 percent of them experience migraines with aura, and only 5% have aura without headache.
Ischemia causes dark and static abnormalities, while migraine auras are usually brilliant and shimmering with a dynamic character. Despite these distinctions, distinguishing between migraine aura’s and amaurosis fugax may be challenging. A migraine aura, according to the International Headache Society (IHS), is a recurring condition that develops over 5-30 minutes and lasts less than 1 hour.
Epidemiology
Transient visual loss is rare all around the world. Adults are more likely than children to have transient visual disruption. Furthermore, the adult etiologic profile varies from that of children.
Women are more likely than males to have medically unexplained visual problems. Griffiths et al found that 79 percent of individuals with medically unexplained vision loss are female and 21% are male. Other medical experts have examined 36 percent of these individuals with unexplained symptoms. Visual function improves with age, illness duration, early therapy, job status, and mental history, although in 42 percent to 44 percent of instances, it fully disappears.
Migraine, a frequent cause of temporary visual loss in people of all ages, affects women more than men. In the United States, females have a 14-18 percent 1-year prevalence of migraine, while males have a 6 percent prevalence, but the female preponderance is not observed until after menarche. Boys and girls suffer from migraines about equally or somewhat more often among youngsters under the age of seven.
Risk Factors
The most significant risk factor for classic ischemic TMVL is carotid artery stenosis, which varies depending on the etiology. Atrial fibrillation, high blood pressure, diabetes, hyperlipidemia, hypercoagulable condition, and myeloproliferative diseases are all risk factors.
TMVL may be caused by a variety of factors, including those listed above, although the most frequent cause is low blood flow to the retina or optic nerve. Low blood pressure, clot, embolus, inflammation of the arteries, or vasospasm may all cause hypoperfusion. Typically, a carotid artery embolus breaks free and temporarily occludes the central or branch retinal arteries, as well as the ocular artery. Reduced perfusion via one or more posterior ciliary arteries is typically the cause of ischemia affecting the optic nerve. TBVL may be caused by the same hypoperfusion mechanism if it is bilateral such as vertebrobasilar ischemia, or it can be caused by the various neurologic or ophthalmic etiologies listed above. It also means that the lesion is anteriorly bilateral, chiasmal, or retro chiasmal.
Diagnosis
Questions must be asked about the patients’ experiences with these events. The initial step is to encourage patients to talk about these four elements of their TMVL.
Monocular/Binocular, If the visual loss occurred in one or both eyes, the examiner should ask. It may be hard for a person to remember which eye it was if it was just in one. Atypical headaches, papilledema, and seizures may all induce transient binocular vision loss (TBVL). Giant cell arteritis (GCA), retinal artery blockage, and thromboembolic events may all induce TMVL. Transient binocular and monocular vision loss may occur with or without ocular health issues. When there are no ocular pathological signs, it’s essential to evaluate the circulatory system using tests including blood pressure monitoring, carotid auscultation, and carotid ultrasonography.
Duration, TMVL episodes may last anywhere from a few seconds to up to s day. It’s possible that a patient won’t remember how long the transient vision loss lasted. In any case, a rough estimate may aid in determining the reason. TMVL associated with migraines has a longer duration and a gradual start, lasting up to an hour.
Papilledema is a bilateral ischemic event that causes brief visual loss lasting one to two seconds.
TMVL caused by thromboembolic reasons may last anywhere from one to fifteen minutes.
Provoked/Unprovoked, what were the patient’s activities at the time of the visual loss, and were there any recent drug changes? TMVL may be triggered by a change in the dose of hypertension medicines. During a rapid postural shift, reduced blood circulation of the optic nerve may cause a temporary dimming of vision. Another example of induced TMVL is a delayed recovery after seeing a strong light source, such as vehicle headlights.
Because of the link between clotting events and vascular diseases, unprovoked bouts of vision loss are usually more worrisome.
Any variables that may have contributed to the vision loss should be identified. Patients with papilledema, for example, may have vision loss as a result of orthostatic alterations. The nature of the problem should be elicited from the patient. Visual abnormalities caused by ischemia, such as amaurosis fugax, are often linked with darkening of vision. Migraine is associated with a number of bright lights.
The patient’s ischemia risk factors, such as a history of high blood pressure, diabetes, or excessive cholesterol levels, should be evaluated as part of the medical history. Questions about a personal migraine history as well as a family history of migraine. It should be considered if the patient has any underlying medical issues like collagen vascular disease, sickle cell disease, or vascular inflammation, or (vasculitis)
A thorough ophthalmologic examination is required (e.g., Hollenhorst plaque, angle-closure glaucoma). In addition, pay close attention to the temporal artery area, looking for soreness or erosions. A thorough cardiovascular exam with a focus on the existence of arrhythmias or a carotid bruit may also be conducted. The majority of AF patients, on the other hand, have normal eye examinations.
There really are no tests that can be used to verify or refute a patient’s claim of temporary visual loss. Furthermore, in individuals with temporary vision loss due to both organic and nonorganic causes, eye test results may be normal. Patients who have symptoms that are medically unexplained are regular visitors. One out of every five new consultations in primary care includes a patient with symptoms for whom no organic explanation has been identified. Despite the prevalence of unexplained symptoms, little study has been done in this area.
A basic laboratory workup should be performed on patients with temporary visual loss (TVL). Blood pressure should be monitored since hypotension is a common cause of vision problems. In the appropriate clinical context, the following blood tests should be considered:
Following an ophthalmologic examination, laboratory tests such as erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) are used to assess for GCA in older individuals. Carotid artery imaging and a heart assessment are usually recommended. Intracranial vascular occlusive disease, brain ischemia, and previous stroke may be detected by neuroimaging (e.g., MRI of the brain) and vascular imaging (e.g., CTA or MRA of the head and neck). If the TVL was bilateral or if the history indicates a seizure, an electroencephalogram (EEG) may be recommended.
An atheromatous plaque at the carotid bifurcation causes a brief decrease in retinal blood flow, resulting in transient monocular vision loss in adults. Since a result, evaluating the carotid circulation in individuals with temporary monocular vision loss is critical, as an early carotid surgical intervention may help avoid stroke. In contrast, there have been no reports of children experiencing temporary vision loss owing to atheromatous carotid illness.
Depending on the patient’s medical history and systemic examination results, echocardiography should be considered.
When a patient’s vision loss is medically unexplained, it’s critical to consider the potential that a subtle pathologic disease is present that was overlooked during the first examination. Electrophysiology should thus be examined to rule out anomalies like Batten disease or Stargardt illness.
Treatment
Migraines
The cause of temporary vision loss (TVL) determines the therapy. Because of the risk of increasing vasoconstriction, certain migraine medications, such as triptans, and beta-blockers, are avoided in migraine-induced temporary visual loss.
The intensity and frequency of migraines determine the treatment. Reducing trigger factors, stress management, and biofeedback are examples of non-pharmacologic treatments. Massage, acupuncture, osteopathic, and chiropractic manipulation are examples of physical treatments that may be helpful in specific situations. For migraine therapy, a variety of transcutaneous (through the skin) electrical nerve stimulation devices is currently available. Acute therapy and preventive therapy are two types of pharmacologic treatment. Simple and combination analgesics, nonsteroidal anti-inflammatory medications, steroids, ergot compounds, and specific triptans (serotonin receptor agonists) are examples of acute treatments. Monoclonal antibodies regulate the calcitonin gene-related peptide neurotransmitter in a highly target-specific manner.
Occlusions of the Retinal Artery
Occlusions of the retinal arteries have no conventional therapy. Ocular massage, hyperventilation by blowing into a paper bag, which may induce vascular dilatation, and decreasing intraocular pressure by paracentesis or medication are all suggested treatments for dislodging the embolus. To be successful, these therapies must be started within 6 hours after the beginning of symptoms. In recent research, intravenous prostaglandin infusion treatment was shown to improve eyesight in individuals with acute CRAO by a statistically significant margin. The goal of treating a patient with a retinal artery blockage is to reduce the risk of stroke and other vascular complications. Statins and aspirin-based antiplatelet treatment are among the medications available. To minimize the chance of another retinal artery blockage or a future stroke, patients are also recommended to manage any underlying high blood pressure and glucose levels, stop smoking and lose weight.
Giant Cell Arteritis
To reduce inflammation and manage symptoms, patients with GCA are typically given high-dose intravenous corticosteroids. AION-related vision loss is a neuro-ophthalmic emergency that requires urgent treatment to avoid impairment and involvement of the other eye. For three to five days, these patients are given 1 to 2 grams of intravenous methylprednisolone. This is followed by a daily dose of 1mg/kg of oral prednisone, reduced over six to twelve months. Although the ESR and systemic symptoms should improve rapidly after the first dose of steroids, the visual prognosis is typically poor. Symptoms may return after corticosteroid treatment, vision loss might worsen even when on corticosteroid medication, and vision recovery is uncommon. Tocilizumab, a steroid-free interleukin-6-receptor antagonist, has been shown in recent trials to reduce recurrence rates.
Optic Nerve Issues
For certain optic nerve issues, surgery is a possibility. Slits are created in the optic nerve sheath to improve CSF (cerebrospinal fluid) outflow and reduce pressure on the optic nerve in optic nerve sheath decompression. CSF diversion is a separate procedure that utilizes a shunt and is more successful at decreasing headaches than vision loss. Treatment for this illness may take months or years. Even after therapy, people may still have papilledema, elevated ICP (intracranial pressure), and visual field abnormalities.