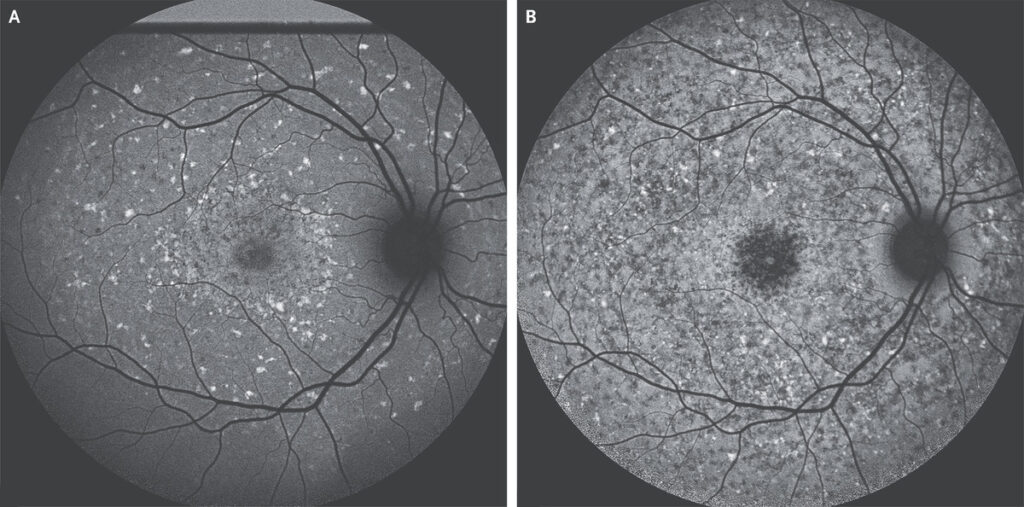
All Macular Degeneration patients begin with early-stage (early) AMD, which is characterized by a lack of symptoms. Drusen, or small white spots in the retina, are detected by eye specialists as people get older. Small “trash” deposits emerge as the retinal cells become less efficient at completing “housekeeping” activities. Early AMD is thought to be caused by oxidative damage and inflammation.
The balance between the generation of highly reactive oxygen-containing molecules that can interact negatively with other molecules inside our cells and our body’s ability to neutralize these chemicals is disrupted in oxidative stress. A variety of factors can produce oxidative stress, including strong light, a poor diet lacking in antioxidants, and too much iron in the retina. The inflammation that results can cause a variety of age-related disorders, such as age-related macular degeneration. Antioxidants are substances found in cells that can stop these damaging processes from happening.
What is the macula?
The Macula is the small portion of the retina that has the densest concentration of photoreceptors, which provides the detailed, central portion of our vision. It’s what enables us to see small precise detail such as to read.
Types of macular degeneration
There are various varieties, some of which are rarer than others. Each variety has its own set of characteristics, and each is treated differently. Wet macular degeneration, Stargardt disease, and myopic macular degeneration are less prevalent kinds of macular degeneration. The most common type is the dry form of macular degeneration.
Dry AMD
Geographic atrophy is another name for dry macular degeneration, which is the other type of age-related macular degeneration. The macular tissue thins and breaks down with time, eliminating the macula’s light-sensitive cells. This weakens central vision, which cannot be repaired or corrected.
Wet AMD
Wet AMD is one of two types of age-related macular degeneration. Wet, exudative, or neovascular AMD accounts for just 10% of AMD diagnoses but 90% of legal blindness. This type of AMD affects central vision when blood vessels leak fluid or blood into the macula. Wet macular degeneration is a late-stage disease.
Stargardt Disease
Stargardt disease, sometimes called Stargardt macular dystrophy or juvenile macular degeneration, is an inherited retinal illness that results in progressive macular degeneration. This form of the disease occurs at a much younger age and is very rare.
Stages of the disease
Subclinical stage of AMD
The early indication of AMD is night vision difficulties, which are subtle but progressive. Impaired dark adaption function is the initial biomarker of AMD, with impairment occurring at a subclinical level at least three years before drusen become evident.
At this time, there are no pigmentary abnormalities visible on examination. When patients have strong corrected visual acuity and the retina appears normal on clinical examination, diagnosing the early stages of AMD can be difficult. As a result, a routine vision test may not reveal any signs or symptoms of the condition.
Intermediate stage
In the early stages of AMD, most people do not feel any negative symptoms or vision loss, however, night vision issues are common. Medium-sized drusen are observed despite the absence of pigmentary abnormalities on inspection.
Advanced stage
The disease is progressive, and early symptoms can quickly deteriorate. Geographic atrophy (GA) or choroidal neovascularization (CNV) causes visual loss at this stage (CNV). This is the stage that is when the disease goes from dry to wet form. The newly formed blood vessels are very fragile and can break or become leaky causing fluid to flood the retinal tissue.
What are the risk factors that cause macular degeneration?
- Age: The most important risk factor for macular degeneration is getting older. The illness affects about 1% of white persons aged 60 to 69, whereas it affects 14% of those aged 80 and up.
- Gender: Women have a slightly higher risk according to studies.
There appears to be a relationship between the start of menopause and the development of macular degeneration. In reality, there is a study into the role of estrogen in the treatment of macular degeneration.
Furthermore, because women live longer than males, they are more likely to experience significant vision loss as the disease progresses. - Genes: Heredity plays a significant role. If an immediate family member has it, your chances are greatly increased, and preventative care should be taken to reduce your chances of expressing the gene.
- Smoking: Smoking is a major cause of macular degeneration. It increases your risk by four times.
- Sunlight and blue light: UV and High-intensity blue light have been linked to being a cause of macular degeneration.
- Medications: Some medications such as warfarin or coumadin have been shown to contribute to the progression of wet macular degeneration. Aspirin and some beta-blockers have also been thought to possibly do the same however it hasn’t been proven yet.
- Race: White Americans are the most affected by AMD
- Eye color: Light-colored eyes have less pigment to protect the other retinal structures from harmful blue light and UV radiation, this can be a cause of macular degeneration also.
- Foods: Processed foods and foods high in trans fats. Tropical oils, like palm oil and coconut oil. Lard and vegetable shortening, and margarine. High-fat dairy foods. Fatty beef, pork, and lamb.
- Cardio vascular disease: Anything that causes a lack of blood flow or oxygen supply to the retina will increase the risk of developing AMD.
Foods that prevent macular degeneration
- Since we know that the main causes of macular degeneration are fatty deposits and oxidative stress. We need to eat foods that help clear the fats, provide anti-oxidants and help with blood flow and cellular health.
- Cooking with vitamin E–rich safflower, olive, canola, flaxseed, and corn oil. Will reduce the trans-fat intake.
- Choose dark green, brilliant yellow, or red vegetables if you want to increase your carotenoid intake. Kale, spinach, collard greens, and broccoli; red and orange peppers and carrots; and maize and sweet potatoes are all good choices. Carotenoids are powerful anti-oxidants.
- Fruits high in Vit C. Vitamin C (ascorbic acid) aids in the formation of collagen, which is necessary for the formation of robust blood vessels in the eyes and elsewhere. Your eyes metabolize nutrients fast, so having enough vitamin C and other nutrients that help eyesight is vital. People at high risk for AMD who take vitamin C, beta-carotene, vitamin E, and zinc may see a 25% reduction in the advancement of advanced AMD and a 19% reduction in the loss of visual acuity (sharpness). Citrus fruits are one of the best sources of vitamin C. Vitamin C is abundant in bananas, apples, and peaches.
- Omega 3’s from fish like herring, salmon, albacore tuna, sardines, and mackerel help to keep the cell walls strong and help to facilitate the pumping of the other vital nutrients into the cell.
- Eggs in moderation, Egg yolks include one of the greatest quantities of the two primary carotenoids that can preserve your macula—lutein, and zeaxanthin.
- Coffee and CLA chlorogenic acid and coffee have 8 times more than just caffeine, CLA is a powerful anti-oxidant.
- Dark chocolate with flavonoids.