Children, teens, and young adults are the most common victims of Stargardt disease. An issue with one’s center vision may be the first symptom. It might be hazy, distorted, or have black patches. The eyesight on the sides (peripheral) is frequently unaffected. Some individuals have difficulty perceiving colors.
Stargardt disease
The most prevalent cause of juvenile macular degeneration is Stargardt’s disease. Learn about the disease’s diagnosis and treatment options.
Stargardt Macular Degeneration
Stargardt macular degeneration is a progressive vision loss condition caused by a hereditary eye illness. The retina, a specialized light-sensitive tissue that lines the back of the eye, is affected by this condition. Stargardt macular degeneration specifically affects the macula, a tiny region at the center of the retina. The macula is in charge of precise center vision, which is necessary for activities like reading, driving, and identifying faces. A fatty yellow pigment (lipofuscin) accumulates in cells underneath the retina in most persons with Stargardt macular degeneration. The aberrant buildup of this chemical over time might cause harm to cells that are necessary for good central vision. People with Stargardt macular degeneration also have impairments with night vision, which makes it difficult to maneuver in low light. Color vision is also a symptom for some people who are afflicted. Stargardt macular degeneration signs and symptoms often occur in late childhood to early adulthood and worsen with time.
Who Does Stargardt Affect?
In the United States, Stargardt’s disease is the most prevalent type of juvenile macular degeneration, affecting one in every 10,000 children. The condition affects both eyes and develops between the ages of 5 and early adulthood, and is named after Karl Stargardt, a German ophthalmologist. Stargardt’s disease is caused by a genetic abnormality that causes the eye’s photoreceptors to perish. Vision loss starts slowly and then accelerates, eventually reducing core vision to the point that an afflicted individual becomes legally blind while maintaining peripheral vision. Stargardt macular dystrophy, juvenile macular degeneration, and fundus flavimaculatus are all names for Stargardt’s disease.
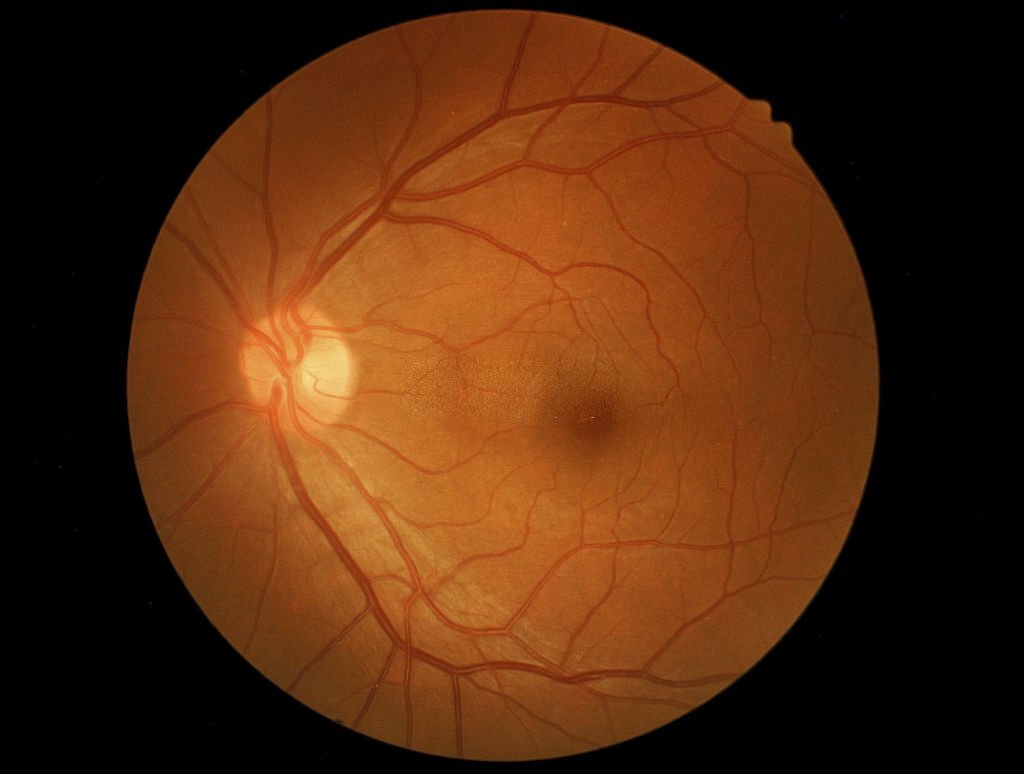
Stargardt’s disease damages the macula, a tiny region at the center of the retina. The macula is in charge of center vision clarity.
Stargardt’s disease is caused by an inherited recessive gene, which means both parents have it. Mutations in the ABCA4 gene are the most common cause.
If both parents carry the gene, their offspring have a 25% chance of receiving it from both parents.
Is Stargardt’s Hereditary?
Stargardt disease is usually handed down from one generation to the next. In order to exhibit symptoms with the typical Stargardt disease, defective genes (the ABCA4 gene) must be handed down from both parents. A person who inherits the gene from just one parent is a carrier for Stargardt disease but does not develop symptoms. Other kinds of Stargardt disease need just one parent’s gene to manifest symptoms, although these are very uncommon.
Stargardt Disease Causes
The ABCA4 gene produces a protein that removes vitamin A metabolites from the eyes’ photoreceptors. Lipofuscin clumps occur in cells lacking the protein, creating yellow clumps in the central retina.
Diagnosis of Stargardt’s disease
After a thorough examination of the retina, an eye doctor may be able to identify Stargardt’s disease. Lipofuscin deposits, or yellow patches in the retina, are often seen in the macula. The yellowish specks come in a ring-like pattern and come in a variety of forms and sizes. A range of eye and vision tests will be used by an eye specialist to confirm a positive diagnosis of Stargardt’s disease.
The tests listed below are useful in determining symptoms: Fluorescein angiography is a test that may be utilized. A dye is injected into your arm during this examination. The dye is imaged as it travels through the blood vessels of the retina. The photographs reveal a black region inside retinal tissue in persons with Stargardt disease. This aids in the diagnosis of Stargardt disease by the ophthalmologist.
Visual field testing evaluates a person’s vision’s whole horizontal and vertical range and sensitivity, as well as scotomas (blind spots), which may be an indication of Stargardt disease. There are a variety of tests available, but none of them are uncomfortable or intrusive.
OCT is a scanning technology that operates similarly to ultrasound. Ultrasound pictures are captured by bouncing sound waves off live tissues, while OCT uses light wavelengths to accomplish so.
Color testing: Stargardt’s is linked to a loss of color vision. The Ishihara test is the most popular way to diagnose color blindness. A succession of colored dot drawings forms the basis of this fast and easy exam. A figure, generally a number, is made up of dots of a distinct hue among the dots. The number will be visible to someone with normal color vision, but a color-blind person would see a different number or none at all.
The inner or rear of the eye is referred to as the “fundus” in fundus photography. The retina, or the very rear of the eye, is seen in a photo of the fundus. In a normal fundus photograph, the optic nerve, macula, and major retinal blood vessels may all be seen. Fundus photography can readily image yellow patches, or lipofuscin, enabling an early Stargardt’s disease diagnosis.
Genetic testing may now be used to determine the kind of macular degeneration that a patient has. This is the most reliable method of determining the genetic cause of your ailment.
What are Stargardt’s disease symptoms?
An issue with one’s center vision may be the first symptom. It might be hazy, distorted, or have black patches. The eyesight on the sides (peripheral) is frequently unaffected. Some individuals have difficulty perceiving colors. Inability to see in low-light situations and having trouble recognizing familiar people. The color vision feature of Stargardt’s may be lost in the latter stages of the disease. The reason for this is that the macula that is affected has cone photoreceptors that are responsible for the color perception of the retina.
Symptoms usually appear in children between the ages of 6 and 12. They may find it difficult to transition from dark to light or from light to dark environments (a condition known as ‘dark-adaptation’). However, some people do not show symptoms until they are adults. People under the age of 20 are more likely to be diagnosed with Stargardt disease. A late-onset variant of the illness may develop in adults beyond the age of 50.
Light sensitivity can also be a symptom of Stargardt’s disease. Bright sunlight, oncoming car lights, wet roads, or bright white lights in the home may be bothersome.
Distorted vision is a common Stargardt’s disease symptom also and may cause people to see things like a door frame that looks curved or wavy or print on a page to me misaligned and wazy. Some of the letters may also be missing.
Disease progression of Stargardt’s
The symptoms of Stargardt disease proceed in a variety of ways. At first, visual acuity (the ability to identify details and shapes) may deteriorate gradually.
Stargardt disease symptoms may appear slowly at first, then pick up pace and level out for some individuals. Vision loss may accelerate at roughly 20/40 visual acuity (meaning what someone sees at 20 feet a normal-seeing person sees at 40 feet). It’s possible that your vision may quickly deteriorate until it’s about 20/200. After this, eyesight tends to remain rather constant.
In certain situations, a person with Stargardt’s (especially the fundus flavimaculatus form of the illness) may not discover visual issues until they are in their middle years.
On a normal eye chart, Stargardt’s disease causes vision loss in the 20/50 to 20/200 range. (Legal blindness in the United States is defined as visual acuity of 20/200 or worse when using corrective glasses.) The fundus flavimaculatus variant of the illness, on the other hand, is associated with much more severe eyesight loss.
While central vision will be impaired, many patients with Stargardt disease will be able to maintain decent side vision for the remainder of their lives. However, since variances may exist even among family members with comparable inherited tendencies, it’s impossible to predict when retinal damage will develop or how quickly it will advance. Patients with Stargardt disease have a broad range of long-term prognoses, which are influenced by their age of onset and genetic variants.
Stargardt’s treatments
Stargardt’s disease is currently incurable and has no therapeutic options. However, various gene therapy and pharmacological treatment experiments are underway. You will know your defective gene as a result of genetic testing, and you will be able to search for and choose to participate in a current study.
Similar disorders have previously been treated using genetic therapies. Stargardt’s disease, too, is expected to be treated shortly, according to doctors.
Astellas Pharmaceuticals is one business working on a therapy for Stargardt’s disease (formerly Ocata Therapeutics). The goal of this stem cell therapy is to preserve and restore photoreceptors in the retina that have been destroyed by eye illnesses such as Stargardt’s. The results of Phase I and Phase II clinical studies were promising, with some patients reporting considerable eyesight improvements.
According to another study, vitamin A aggregation or “clumping” in the retina may be linked to both Stargardt’s disease and age-related macular degeneration (AMD). Vitamin A dimers are clumpy deposits of vitamin A.
Several pharmaceutical firms are working on medications to combat the issues caused by vitamin A dimers. Alkeus Pharmaceuticals‘ ALK-001, for example, is a modified version of vitamin A that produces much less waste when processed in the retina. It is now through Phase II studies.
People who are adapting to visual loss might benefit from a variety of options. Special equipment, practical ideas for everyday life, and training to assist you in getting around are examples of these. Request assistance from your optometrist in locating low vision services.
Your eye doctor may also recommend that you wear eyeglasses with specially tinted lenses to filter particular wavelengths of light if you have Stargardt’s.
By their early twenties, many patients with Stargardt’s disease have lost their vision. The emotional toll of a handicap may be severe, affecting crucial parts of one’s life such as job and social life. Counseling and occupational therapies are often included in treatment plans due to the high level of assistance required.
Handheld magnifiers, reading machines, and video magnification equipment are examples of low vision aids that may assist individuals with everyday activities and chores. All of these aids are designed to help people preserve their freedom.
Special educational needs (SEN) help is available in schools for children with vision loss. This may give your kid the necessary adjustments, equipment, and assistance to fully participate in the program.
Preventing Progression of Stargardt’s Disease
Smoking is not recommended for those with Stargardt’s illness, nor should they be exposed to cigarette smoke. Furthermore, some research suggests that consuming too much vitamin A may aggravate the illness. While vitamin A in meals is OK, excessive dosages of it as a supplement should be avoided.
Sunglasses may assist with Stargardt’s disease’s sensitivity to strong light. Sunglasses may also protect the retina from additional damage caused by the sun’s damaging ultraviolet (UV) radiation.
Life with Stargardt’s Disease
Unfortunately for those who have to deal with this vision-robbing disease, it will definitely make for some life challenges. Luckily it isn’t a lights-out, total blindness disease and there are many low vision devices that can help people do the activities and keep their independence. If you or a loved one need help consult your eye doctor for low vision resources and join some of the online support groups that are available such as on Facebook. Take advantage of the new wearable technologies and stay positive!