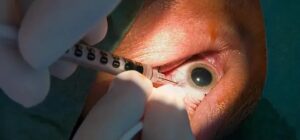
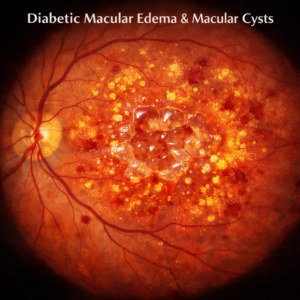
Rare diseases affect fewer than 1 out of every 2,000 individuals and may have serious repercussions that negatively impact vision and bodily functions.
AEVR recently hosted a congressional briefing focused on less-common eye diseases that still impact many patients. Ben Shaberman provided insights about advances in inherited retinal disease while Dan Ignaszewski discussed Thyroid Eye Disease impacts.
Anophthalmia
Anophthalmia is a birth defect in which one or both eyes are absent at birth, creating severe eye malformation that can seriously hinder development and functioning of both the eyes and face. It often co-occurs with other birth defects as well as mutations of specific genes; inheritance may play a part; environmental factors during gestation like medications or infections a mother might have contracted may also have had an influence; doctors can detect anophthalmia during fetal ultrasounds as well as amniocentesis/chorionic villus sampling to obtain samples of DNA and conduct genetic tests in some cases to further investigate genetic testing results.
Anophthalmia symptoms include small boney orbits, short eyelids, reduced palpebral fissure or malar prominence and narrowing of the skull socket. The condition can either affect one eye only (unilateral) or both at once (bilateral).
Individuals living with Anophthalmia need special care and consideration in order to have an enhanced quality of life. Treatment should focus on cosmetic improvements, decreasing risks associated with health conditions and helping daily tasks. Prosthetic eyes have become more realistic, comfortable and advanced to meet these individuals’ needs – children will require time, patience and humor in order to adjust to wearing and caring for their prosthesis.
Anophthalmia can often be detected with genetic tests such as DNA Labs India’s Micropthalmia/Anophthalmia/Coloboma Spectrum Test. This can give valuable insight into its causes, helping families make informed decisions regarding their child’s health and wellness. Our test can be taken conveniently at home at an affordable price – visit our online shop for more information or to place your order.
Retinitis Pigmentosa
Retinitis pigmentosa (RP) is an inherited condition in which light-sensitive tissue in the back of the eye (the retina) begins to break down over time, leading to progressive vision loss and eventually blindness. Because different genetic mutations cause different forms of Retinitis Pigosa, symptoms will vary greatly from person to person and symptoms may not show themselves right away.
Early signs of Early Onset Blindness in children include poor night vision, difficulty seeing in dim or dimmed light conditions and eventually tunnel vision. Over time this condition may also lead to loss of peripheral (side) vision and eventually blindness.
Sometimes mutations of genes are passed from parent to offspring; other times they can occur randomly. Some forms of the disease appear as part of another health condition (Usher syndrome or Leber congenital amaurosis for instance), while other times they stand alone as distinct conditions.
Researchers are exploring gene therapy, stem cell therapy and electronic retina implants as potential solutions to slow the progression of RP; however these approaches remain experimental at best. If your family history includes the condition be sure to discuss genetic testing with your physician as soon as possible for personalized advice and counseling.
At present, regular doses of Vitamin A palmitate and decosahexaenoic acid (DHA), under medical supervision, is currently the best approach for managing retinal pigmentary (RP). This supplement can help prevent macular edema – an often-complicated side effect of RP – as well as improve night vision; but will not stop its progression. If any symptoms arise that could compromise vision or interfere with night driving skills, see your physician immediately; they may suggest other therapies, including Acetazolamide which might help slow its development if necessary.
Bell’s Palsy
Bell’s Palsy, commonly referred to as facial nerve palsy, is characterized by sudden weakening or paralysis of the seventh cranial nerve – commonly referred to as the facial nerve – on one side of the face, often leaving one side appearing droopy and can affect people of all ages. While symptoms typically resolve within several weeks and some even see full recovery within six months.
This disorder is believed to be caused by herpes virus, which lies dormant within our bodies until activated, leading those with compromised immunity – including diabetes patients, high blood pressure individuals, those suffering upper respiratory infections and pregnant women – more prone to this condition.
Bell’s Palsy symptoms include inability to smile on one side of the face, closed eyes, loss of taste and other associated discomforts such as earache, sound sensitivity on affected side and difficulty closing eye on affected side. While most patients with Bell’s Palsy will recover over time, treatment often includes physical therapy sessions, medication or injections of corticosteroids or antiviral drugs in an effort to speed recovery times.
Bell’s Palsy patients typically make a full recovery; however, some may experience persistent symptoms. If this occurs it is important to see an ophthalmologist so as to rule out other potential causes, including stroke. Once confirmed as not due to stroke then treatment could involve weight management, exercise and sleep habits as possible causes. Ideally eye lubricants are also often recommended as this helps protect the cornea and avoid potential damage from occurring.
Anopthalmia and Micropthalmia
Microphthalmia or anophthalmia refers to birth defects where one or both eyeballs are either missing, abnormally small, or both are missing altogether (microphthalmia or anophthalmia). These birth defects result from changes to certain genes during crucial prenatal development and may occur as random mutations (sporadic) or be genetic (congenital). Microphthalmia and anophthalmia belong to a group known as the MAC spectrum, in which mutations of multiple genes involved with normal ocular development cause these malformations.
People suffering from this condition may also suffer other eye issues, including dimness or cataract. Furthermore, missing pieces of tissue could be present in structures of their eyes such as notches or gaps on structures such as an iris (colored part of eye) or light-sensitive tissue lining back of retina (choroid). Finally, optic nerves connect eyes to brain.
Anophthalmia or microphthalmia caused by gene mutations often occurs as part of a syndrome affecting other areas of the body, including skeletal defects, heart disease, intellectual disability or seizures – known as syndromic anophthalmia and more likely than isolated cases.
Doctors can often detect eye defects before birth with prenatal tests such as ultrasound and genetic screening or at birth through physical exams and physical exams after birth. Doctors can also use X-ray or computed tomography (CT scan) scans to detect some birth defects that arise after birth, including anophthalmia. An early diagnosis allows doctors to treat anophthalmia with various devices that allow other parts of their face to grow normally such as prosthetic eyes. A knowledgeable ocularist may assist in creating such devices while working alongside an experienced oculoplastic surgeon in correcting their socket so their prosthetic can fit better.
Glaucoma
Glaucoma occurs when fluid pressure in the eye increases and damages the optic nerve, and is the second-leading cause of blindness among both humans and animals. It typically starts off slowly by diminishing peripheral (side) vision before progressing to total blindness if left untreated.
Primary open-angle glaucoma, the most prevalent type of glaucoma, typically manifests gradually and without pain. Here, eye fluid doesn’t drain properly from its system (similar to having a blocked drain), leading to increased eye pressure that eventually damage its optic nerve over time.
Closed-angle glaucoma, which may be more severe than open-angle glaucoma, occurs when drainage areas in the front part of the eye become blocked and eye pressure rapidly rises, leading to symptoms including eye pain, blurred vision, rainbow halos around lights and nausea. Treatment includes beta-blockers, alpha-adrenergic agonists and prostaglandin analogs; surgery may also be used to stop or delay progression of this form of the disease.
If you have glaucoma, it is essential that you visit an ophthalmologist regularly. At these visits, he or she will conduct tests for signs of the condition as well as take measurements such as tonometry (a measure of pressure inside the eye) and Pachymeter thickness measurement testing as well as taking photos with an OCT machine (Pentacam). Your doctor may give eye drops to dilate pupils temporarily blurring your vision – or, in extreme cases, prescribe other types of medication altogether – should they not find anything relevant for treating their condition glaucoma symptoms.