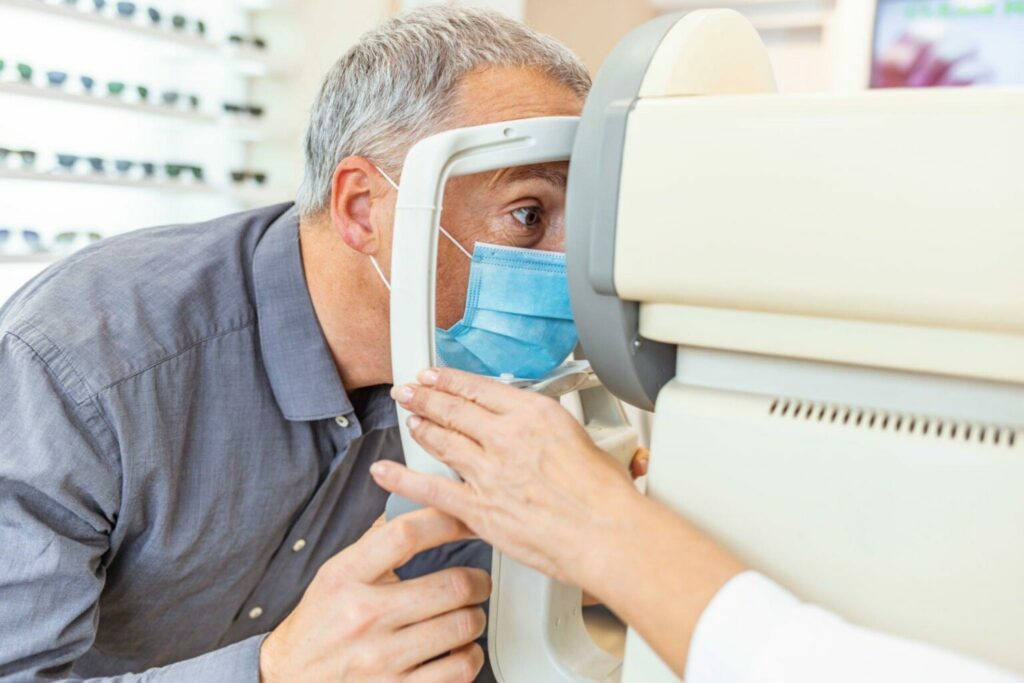
Can macular degeneration cause visual hallucinations?
Some people have been known to perceive faces or things that aren’t actually there as a result of vision loss brought on by age-related macular degeneration (AMD) or other reasons. But according to a recent study, many more patients with AMD than previously believed have these hallucinations, also known as Charles Bonnet syndrome.
The study discovered that more than 12% of persons with AMD have visual hallucinations. The true figure could potentially be higher. People often have these hallucinations for three years, on and off. Individuals who have hallucinations frequently perceive a variety of visions, including faces and people.
Many people are reluctant to discuss these phantom visions for fear of being diagnosed with dementia or another mental illness. Because they were reluctant to speak up, hallucinations were formerly regarded to be a very infrequent occurrence.
Because of the decreased amount of regular visual information arriving from the eyes, the brain effectively manufactures these hallucinations. The duration of the intricate visuals, which can last anywhere from a few seconds to several hours, can range from seconds to completely formed representations of animals, artwork, faces, or landscapes. People are hesitant to discuss their hallucinations because they believe it implies that they have a mental disorder or are “going crazy.” Instead, it is really a typical side effect of poor vision.
Charles Bonnet syndrome patients are aware that the pictures they are seeing aren’t real. On the other hand, those who suffer from psychiatric disorders may have delusions in which they think the hallucinations they perceive are genuine. Hearing voices may also be related to these disorders (mental illness).
Phantom limb syndrome is comparable to Charles Bonnet syndrome. Because the brain’s sensory cells continue to fire signals even in the absence of the affected limb, amputees with this syndrome nonetheless “feel” their severed limbs. Similar to Charles Bonnet syndrome, when the brain’s visual center doesn’t get information from the macula, it replaces illusions.
How to handle macular degeneration hallucinations?
Charles Bonnet syndrome has no known cause or therapy, although there are ways to prevent episodes and manage hallucinations when they do happen.
Get in touch with your physician or ophthalmologist if you believe you are seeing things that aren’t actually there. They will rule out other potential sources of visual hallucinations, such as neurological disorders or adverse drug reactions.
Your doctor will teach you methods to control the hallucinations if they believe you have Charles Bonnet syndrome. These consist of:
- Changing the environment and illumination in which you work
- blinking often or quickly shifting your gaze from side to side while maintaining your head in one position.
- Sleep, exercise, or relaxation are all recommended since weariness and stress can make hallucinations worse.
If you have macular degeneration hallucinations, try the following exercise:
Imagine two locations on a wall in front of you that are left and right approximately a meter (3 feet) apart. For 15–30 seconds, a glance from one spot to the other once per second or faster while standing approximately a meter and a half away. When gazing left and right, keep your eyes open and your head still. Pause for a moment.
Try doing the exercise again if your hallucinations persist.
The method probably won’t work if they haven’t quit after four or five tries. However, you might want to give it another go at a different time or for a different kind of hallucination.
Additional methods for stopping a hallucination include:
- Close your eyes or turn away from the image.
- Turn on the lights in the room or, if you’re in a highly lit place, choose a darker location.
- Simply stand up and carry out another task.
- The hallucinations may stop as a result of this, but they frequently return.
By emphasizing that the symptoms patients are experiencing are a result of their visual deterioration and not a reflection of their mental health, ophthalmologists may reassure and assist patients.
What do hallucinations with macular degeneration look like?
Simple unformed bursts of light, color, or shape are a common symptom of Charles Bonnet’s hallucinations.
However, many people see more complex shapes like lattices and geometric grids.
Some CBS users claim to have observed manicured views or gardens, creatures, humans, the procession of tiny dressed people wearing caps, or even disembodied faces with fixed gazes. Often, the hallucinations are more vividly detailed than the real world.
Some people actually like their hallucinations. However, they can be terrifying and are more frequently an unpleasant distraction.
They may also obstruct normal eyesight.
Additional therapies for Macular Degeneration Hallucinations
Some people can stop hallucinations when they happen, while others require additional assistance.
Treatments are being created and are already available.
Hallucinations that are really upsetting can sometimes be treated with medicine. These drugs have been demonstrated to be effective for Charles Bonnet’s hallucinations even though they are often recommended for different diseases. In order to prescribe them and do additional tests to determine their safety and rule out other potential causes of hallucinations, a specialized doctor would often be needed.
It’s critical to create novel hallucination therapies. The Macular Society has funded research at Newcastle University under the direction of Professor John-Paul Taylor to determine whether visual hallucinations brought on by Charles Bonnet syndrome may be curbed by gently applying an electric current to the scalp at the rear of the head.
Transcranial direct current stimulation is the method’s name (tDCS).
There aren’t many, if any, negative effects, according to preliminary data, and it may help reduce the frequency of hallucinations. However, further studies are required to prove this.
Which tests are used to diagnose hallucinations with macular degeneration (CBS)?
For CBS, there are no particular exams. Your doctor will certainly suspect CBS as the cause if you have visual hallucinations. An eye exam and various neurological and cognitive tests may be performed in order to make the diagnosis. This is done to rule out a few other illnesses that might also result in visual hallucinations (see below). In addition to visual hallucinations, these additional illnesses typically present with other symptoms.
What further diseases resemble Charles Bonnet syndrome?
Simple visual hallucinations, such as flashing lights or zigzag patterns, can also be caused by the following conditions:
- Eye conditions such as retinal detachment, glaucoma, retinitis pigmentosa, and retinal vein or artery occlusions. Any eye disease that results in permanent vision loss.
- Conditions that impact the ocular nerves (for example, optic neuritis).
- Diseases that impact the brain’s visual cortex (for example, migraine, epilepsy, brain tumors).
Conditions that can cause complex visual hallucinations, frequently in vivid color and dramatic form:
- Dementia, especially dementia with Lewy bodies. Common forms of dementia like Lewy body dementia frequently result in hallucinations. Other signs include:
- Memory, judgment, focus, and recognition changes (more than would be expected for your age).
- Symptoms of tremor, slowness of movement, and stiffness.
- Falls, sleep disruption, and drowsiness is other frequent symptoms.
- Parkinson’s disease. This frequently results in melancholy, tremors, rigidity, and slowness. Hallucinations involving images are uncommon.
- Epilepsy (complex focal seizures).
- Serious mental illnesses like schizophrenia (psychosis). People exhibit additional symptoms of disrupted thinking processes under these circumstances. Typically, they have a strong belief that the visual hallucinations are genuine (and often experience associated sound and smell).
- Drug abuse, especially with regard to opiates like heroin and hallucinogens like “magic mushrooms” and LSD. Complex hallucinations, which can be quite unpleasant, may be brought on by them.
- A stroke may result in CBS if it results in an abrupt loss of vision or if it affects the midbrain. Sound or scent is typically absent from the visuals.
- The uncommon illness known as Alice in Wonderland syndrome is most frequently observed in children who have brain inflammation, as a result of certain medications, or who have certain types of migraine. Objects look bigger or smaller than they actually are because of the condition.
While CBS only consists of visual hallucinations in persons with limited eyesight, these diseases can be distinguished by other factors.
What is the prognosis for those with macular degeneration and hallucinations?
CBS often doesn’t stay forever. The visions often linger for around 18 months before starting to fade. It is thought that this occurs because the brain adjusts to having limited eyesight. Five years following the onset of the symptoms, a recent study indicated that although the majority of participants saw a decrease in their frequency, they continued to sometimes have hallucinations.
Conclusion
Patients with low vision should be informed about macular degeneration hallucinations or Charles Bonnet syndrome.
According to research, patients with low visual acuity are more prone to suffer the defining symptoms of Charles Bonnet syndrome, such as phantom vision or visual hallucinations.
Charles Bonnet syndrome was seen in 87 low-vision participants (34%) but in just four control subjects (1.6%), out of 258 low-vision subjects and 251 matched controls with little to no vision loss. Individuals with visual acuities between 20/301 and 20/800 had a twofold increased risk of developing the visual abnormalities associated with Charles Bonnet syndrome compared to patients with other visual acuities.
The most frequent cause of reduced vision was age-related macular degeneration, although there was no statistically significant variation in frequency according to the reason.
Patients reported experiencing episodes between one and thirty times a month on average, although only eight out of 87 participants (9%) said they sought medical attention. Only half of those who sought medical advice believed they received an explanation for their problems. The most frequent times for episodes were said to be between 6:00 a.m. and 12:00 PM and between 6:00 pm and midnight.
The current study’s findings indicate that there is no need for therapy, but it is crucial that ophthalmologists and their staff thoroughly explain Charles Bonnet syndrome to patients and reassure them that it is a common condition.
FAQ’s
What results in the Charles Bonnet syndrome-related hallucinations?
Loss of eyesight is associated with Charles Bonnet syndrome. Your brain receives less information from your eyes than usual when you lose sight. Sometimes, your brain compensates for this by producing hallucinations.
What causes hallucinations the most frequently?
Mental health problems like schizophrenia or bipolar disorder are common causes of hallucinations. drinking and drug use. Parkinson’s disease or Alzheimer’s disease.
What area of the brain is impacted by Charles Bonnet syndrome?
Visual hallucinations develop as a result of impairment along the visual pathway in Charles Bonnet Syndrome.
What may result in unexpected visual hallucinations?
Visual hallucinations can have a variety of etiologies, such as retinal disease, migraines, acute stroke, medication-related side effects, neurodegenerative disease, alcohol or drug use, toxic-metabolic encephalopathy, and mental disorders. There are two types of visual hallucinations: basic and complicated.
Does Charles Bonnet’s syndrome reappear or disappear?
In contrast to mental images, Charles Bonnet’s hallucinations seem to exist in the physical world. They appear and disappear suddenly, and their durations range from a few seconds to a day or longer. The actual Charles Bonnet syndrome might endure for a few hours to several years.
Who type of doctor treats Charles Bonnet syndrome?
A low-vision eye doctor or a retinal specialist can provide support and assistance for those with low vision. After a person has a visual loss, Charles Bonnet syndrome (CBS) may manifest.